To create and send an invoice intended for processing using Patient Claims
1. Ensure you have selected Invoices as the view option. Issue a new invoice and select it, or select an existing invoice to process using Online Patient Claiming.
2. Ensure you have selected Invoices as the view option, and click the Patient Claim button (from the Accounts window). The New Patient Claim window appears.
3. Click the View Invoice Items button to view the invoice items included in this claim.
13 If you choose to cancel a Patient Claim in the course of processing the claim, the following message displays:
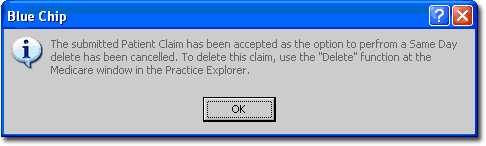
Notes on Patient Claims
o Invoice items must be receipted correctly to be eligible for Patient Claiming. Acceptable receipting methods will be:
o All invoice items are unpaid – that is no receipt has been issued.
o All items are partially receipted – each invoice item in the invoice must be partially paid. Receipting in this manner has implications to Medicare in respect of the "Safety Net" calculations, and the capacity to pay benefits to the Practitioner and the Patient in the same claim.
o All items are fully paid – that is the invoice is fully paid.
o Invoices can include the non-Medicare item MISC, but no other items from non-Medicare lists.
o Invoices must have at least one service item that has a non-zero amount.
o Non-MBS items contained in an invoice cannot have a zero amount.
o The Patient must have a valid and current Medicare card to make a Patient Claim.
o Standard referrals used for Patient Claims invoices must have the referring Doctor's provided number recorded.
o Once an invoice has been attached to a patient claim, it cannot be attached to a second patient claim unless the previous claim has been deleted or "Same Day Deleted".
o Invoices cannot be adjusted or deleted once they are attached to a Patient Claim.
o If a Patient Claim already exists for the selected invoice, the Patient Claim window will be opened in "view" mode.
Notes on Sending Invoices When Using Online Patient Claims
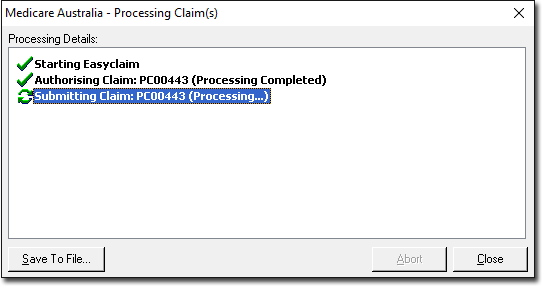
o Once the Patient Claim transmission process has begun, the "Abort" button will be disabled. Due to the nature of the Patient Claim communication, it cannot be interrupted during the process.
o The processing dialogue will be closed automatically once a claim is successfully transmitted or stored.
o A stored claim will validate and authorise the claim only. No transmission to Medicare will take place in the storing phase.
o A Lodgement Advice must be printed for successfully created store and forward claims, or for immediate claims referred to a Medicare Operator.
o A Statement of Claim and Benefit must be printed for successful immediate claims.
o If claims are rejected on the basis of incorrect Medicare card information for the Patient or Claimant, the relevant details must be updated in Bluechip prior to resubmitting the claim.
o Unsuccessful claims will be deleted in Bluechip to allow for the invoice to be resubmitted with another Patient Claim. These claims will not appear in the claims list – their deletion is absolute. Note: once an Invoice has been attached to a Patient Claim it cannot be attached to another Patient Claim unless the first claim is deleted. This is the same as BB/DVA claims. This is to stop the possibility of Invoices being submitted twice.
o A Patient Claim can reach the following statuses during the transmission process:
• Submitted
• Report Received
• Successful
• Pending
• Rejected
o As each claim status has been achieved, Bluechip will record the date and time at which this occurred.
o When a Patient Claim has been created using the Store and Forward option, its status is "Awaiting Transmission". Only claims with this status can be submitted using the Store and Forward process.
o No reports are required as a result of transmitting a Store and Forward claim.